Claim denials can have a significant negative impact on a medical practice, and the management of these denials remains an essential component of any solid revenue cycle plan. It is important to point out that this involves more than just resubmittals and appeals; practices should aim to prevent as many denials as possible from the start and then efficiently manage the ones that could not be prevented. In this article, I will discuss how grouping denial codes can provide valuable data that can be used to adopt a prevention-focused claim denials management process.
Methods for Grouping Denial Codes
The first step of a successful claim denial management approach is understanding the reason for a denial. When claims are returned unpaid, the insurer will indicate the reason on the accompanying explanation of payment. These indicators are known as claim adjustment reason codes (CARCs), or denial codes. There are hundreds of CARCs that can be applied at the claim level or line-of-service level and grouping these codes can provide you with important insights into potential process gaps.
There are several ways that you can group denial codes for review. The following are some of the most common methods:
- Practice Setup. This grouping should include any codes related to taxonomy code errors, provider/procedure code mismatch, facility/procedure code mismatch, etc.
- Department. This group of codes will tie back to specific departments. For example, if expenses occurred prior to the date of insurance coverage, this should have been identified by the department that performed the eligibility and benefit verification services.
- Focus Area. Perhaps your practice is focused on improvement in a particular area, which is a situation that would require you to target a very specific set of codes. For example, if you have set up a new process regarding referral management, you may want to track denials related to “exceeded referrals” and “absent referrals” to gauge performance and set goals for the new workflow.
You may want to consider maintaining 2 sets of grouped codes for review: a “regular” set and an “as needed” set. The “regular” set provides a consistent cadence of insights into performance so you can make adjustments if you see downward trends. The “as needed” set provides the data with which to implement evidence-based decisions as your practice grows and evolves. Examples of both types of sets are listed below:
- Missing Information. This can be an important “regular” grouping to review, as it can help to identify the following:
- Procedures that routinely require prior authorization. Once these are identified, your team can begin to obtain these approvals ahead of procedures to accelerate payment.
- Services that always require visit notes. These can be flagged in the clearinghouse as a submission requirement, or in some cases, automation can be implemented that would attach documentation to claims billed with these service codes.
- New payer trends requiring additional documentation for certain services, diagnoses, or providers.
- Provider Setup. This can be an important “as needed” grouping to review when you are adding new providers. It can indicate taxonomy issues, service/code mismatches, etc.
Applying Data as Part of Your Claim Denial Management Strategy
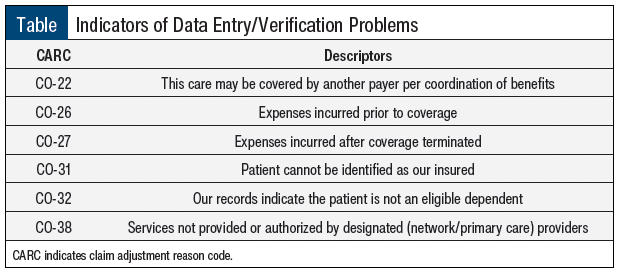
One of the most effective ways to manage claim denials is to prevent them before they occur. The knowledge you obtain from grouped denials can be valuable for reworking processes and reeducating or retraining staff as needed. For example, having a regular grouped review of CARCs specific to data entry/verification can highlight issues occurring at the front desk or with other intake staff responsible for these tasks (see Table).
Leverage your practice management system and clearinghouse reporting capabilities to examine the data in this grouping. Once you have this data you can do the following:
- Review how your facility matches up against industry benchmarks
- Identify improvement processes by reviewing existing processes that could lead to these denials. For example:
- What are your current eligibility verification processes?
- How do you currently obtain patient information and insurance information?
- Do you verify accuracy of data entered against the scanned cards in the system?
- Create new processes to prevent similar denials going forward. For example:
- Automate. When possible, use technology to support you. Can your system identify a patient record from the mobile number he or she called in on?
- Verify Patients. Every patient, every time, as well as their current information. The questions do not have to be complicated. For example, you can ask them to confirm their home address or the last 4 digits of their phone number.
- Set new goals for the rates of denials with CARCs to focus on decrease
- Engage staff in reducing these types of denials to prevent them from recurring. In other words, reward accuracy. Create metrics by which entry staff can be evaluated and rewarded for improved performance.
When it comes to denial prevention, chances are you are going to be working closely with the intake staff because “92% of denials come from data-entry errors made by front desk staff.”1 Therefore, having a static list for front-entry–related denials is a great idea, and sharing it with your front desk workers on a regular basis is an even better idea. Once you have obtained the data to review, you can use it to help your staff by providing training/education, technology automation, and support.
Conclusion
Establishing a robust claim denial prevention process is crucial for running a successful practice. Grouping denial codes is an important component of this process, allowing you to review revenue cycle performance. When this strategy is deployed effectively, it can reduce the time needed for analysis, provide quick indicators of trouble areas, and inform decision-making for you and your staff.
Reference
- McCutcheon D. 3 reasons why billing staff relies on accurate information from the front desk. July 18, 2018. https://blog.accountmattersma.com/3-reasons-why-billing-staff-relies-on-accurate-information-from-the-front-desk. Accessed February 14, 2021.