The US healthcare system has undergone seismic changes in the past several years. Beginning with the Medicare Prescription Drug, Improvement, and Modernization Act of 2003 to the Medicare Access and CHIP Reauthorization Act (MACRA) of 2015, the current focus or priority of healthcare payers has shifted from paying for volume to paying for value. Although the long-term effects of these changes are difficult to conceptualize, the passage of the Affordable Care Act (ACA) of 2010 and then of MACRA are likely to be the most significant milestones of the US healthcare reform since the passage of the Social Security Act of 1935.
The US healthcare system is the largest purchaser of healthcare services in the world, with spending exceeding $3 trillion annually. Dynamic research and development, increasing US life expectancy, and the volume of baby boomers who are retiring are putting considerable strains on the economic viability of the current healthcare system.
Payers, under increasing pressures from different sectors, are searching for the right answer to this looming crisis. Individual payers had been experimenting to define their own models, criteria, and policies to define value and pathways until the passage of the ACA, which is when Medicare—the largest payer for healthcare services in the world—initiated the Hospital Readmissions Reduction Program, along with a number of incentives and penalties, which is a monumental change that began penalizing hospitals for readmissions within 30 days of hospital discharge and is a leading healthcare cost driver.
MACRA is the first systemic attempt to define value in the delivery of healthcare. Before the passage of MACRA in 2015, the existing system of payments encouraged volume-driven care over value-driven care. Physicians, hospitals, and other providers frequently opted to deliver an ever-higher volume of drugs and services without a corresponding analysis of the effect that these drugs and services had on the quality of care. Multiple research articles and publications showed that more services and higher spending did not necessarily result in superior results and outcomes; in fact, they frequently produced the opposite effect.
Carolina Blood and Cancer Care Associates
The Carolina Blood and Cancer Care Associates (CBCCA)’s physicians and administrators foresaw the changes in the US healthcare system in the early 2010s and began planning for a future that would help them embrace the coming changes rather than wait until the changes were forced on them. In this article, we share our journey of transforming from delivering high-volume and resource-intensive care to a practice defined by delivering value and quality.
The CBCCA leadership began its transformation by engaging with multiple payers and patient advocacy groups to become an active partner in defining the shift from volume to value. We reached out to the Department of Health & Human Services (DHHS) of South Carolina, as well as to our largest commercial payer partners about their perception of the upcoming changes, and explored several possible routes that would allow us to take a lead in carving out a meaningful path toward value-based delivery of care that would benefit all stakeholders—first and foremost, our patients.
After a series of meetings, we decided that our most efficient course of action was to transform our practice into a patient-centered care center. We consulted with BlueCross BlueShield of South Carolina (BCBSSC) and DHHS of South Carolina, and decided to obtain Patient-Centered Specialty Practice (PCSP) accreditation by the National Committee for Quality Assurance (NCQA).
Our leaders, along with BCBSSC representatives, attended a training session in Baltimore, MD, in the summer of 2013 on the PCSP transition process. Although our first impression was that transforming our practice into a PCSP would be a mammoth task, after intensive review of the transformation process, we decided to begin with refining our internal processes and to receive input from stakeholders as we moved on to the next step.
CBCCA Transformation Process and Status
The goals of the transformation included providing patient access to the clinic 24 hours a day, 7 days a week, whether to get injections, speak with their physicians, or to access their medical records.
In addition, we aimed to leverage technology to improve the flow of information and to provide the most efficient and highest-quality care possible.
Furthermore, we wanted to provide medical counseling, injections, and chemotherapy, as well as all other relevant care to improve patients’ overall quality of life. Finally, we aimed to prevent unnecessary emergency department visits and hospitalizations.
After a series of internal meetings and discussions in the summer of 2013, along with input from stakeholders, including BCBSSC, DHHS of South Carolina, and experts from the Community Oncology Alliance (COA) and the American Society of Clinical Oncology (ASCO) to prepare a navigation map, the CBCCA team began its practice transformation.
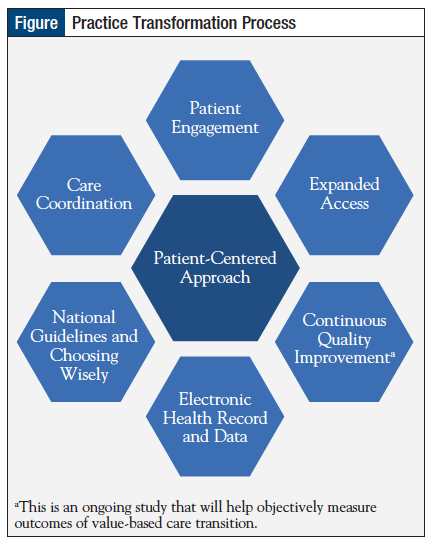
The Figure outlines the steps we took to transform our practice. The process was divided into 6 core areas, with the goal to improve coordinated care and to fulfill the requirements of the criteria, which led to our recognition as a PCSP by the NCQA. The 6 core areas described below include “patient engagement,” “expanded access,” “continuous quality improvement,” “electronic health records (EHR) and data,” “national guidelines and Choosing Wisely,” and “care coordination.”
As part of the practice transformation to patient-centered care, our cancer clinic and infusion services had a well-built foundation and included many of the Centers for Medicare & Medicaid Services (CMS)’s Oncology Care Model (OCM) practice requirements. These changes aligned with our philosophy of incorporating population health management strategies to optimize clinical effectiveness and efficiency.
Core Areas of Practice Transformation
Patient Engagement
Patient orientation and education
We documented our policies and procedures on new patient education and communication standards to ensure timely and comprehensive communication with patients and their caregivers. In addition, we provided educational materials to patients and their caregivers before chemotherapy. We also documented our policies and procedures on a patient callback policy, including medication adherence rates.
Financial counseling
We documented our policies and procedures on financial counseling. We provided accounting logs of financial or drug replacement assistance given to patients. We also secured a robust system to utilize patient assistance and drug replacement programs to ensure care for underinsured or uninsured patients.
Shared decision-making
We present our patients with individualized goals for their care, especially distinguishing between palliative and curative treatments. We also provide patient education and financial counseling.
Secondary prevention and lifestyle modification
We hired a dietitian to provide dietary and nutritional counseling for our patients. In addition, we have a robust smoking-cessation program. As we move forward, we will incorporate a health coach to provide lifestyle modification counseling to patients. In addition, we provide patients survivorship plans and surveillance according to the National Comprehensive Cancer Network (NCCN)/ASCO guidelines.
Advance care planning
One of our physicians completed a certificate course on hospice and palliative medicine, and another physician became a trainer in Education in Palliative and End-of-Life Care. We then started to provide in-house palliative care, advance directives planning, and early intervention of hospice and end-of-life counseling.
Patient experience
We started to collect patient feedback on care using the Consumer Assessment of Healthcare Providers and Systems survey from COA.
Expanded Access
Patient navigation
We now provide same-day appointments for new patients as requested or medically required. We also maintain a monthly log of new patient scheduling procedures that reflects our new triage process, provider requests, and same-day appointments; we are establishing a monthly log of patients who utilize the triage system and after-hours care. In addition, we have 6 certified oncology navigators.
Same-day services
Appointments and walk-ins are offered as a standard part of our practice’s scheduling processes. We documented the process to ensure that all staff members adhere to the appropriate protocols for scheduling appointments based on patient needs.
24/7 access
The on-call physician is available by phone or by web-based EHR system, 24 hours a day, 7 days a week. The triage process for new patient referrals uses the EHR system.
Weekend hours and infusion services
We revised our policies in 2014 to provide expanded access to improve care coordination and communication with referring physicians, and to reduce emergency department visits and hospitalizations. We began providing weekend infusion services in January 2016.
Uninsured and underinsured patients
We provide equal access to patients, regardless of their insurance status. All patients and families receive information regarding the ACA and access to drug services through various foundations. We have successfully found financial resources for 99% of our uninsured patients.
Continuous Quality Improvement
We decided to measure call volume (after hours) after implementing the policy of same-day appointments. We noticed a significant reduction in the number of patient calls. We will be measuring the relationship between same-day appointments and emergency department visits and hospitalizations as an ongoing continuous quality improvement measure.
Care Coordination
Care coordination within the practice
Comprehensive individual care plans are finalized by the oncologist once staging is complete. During this process, the goals of care are discussed, defined, and shared with patients and their caregivers. This information is also shared with all employees involved in patient care, including registered nurses and medical assistants (will be shared going forward with navigators and social workers). All patients are encouraged to follow the “call me first” policy and speak to a triage nurse to avoid unnecessary emergency department visits or hospitalizations. A board-certified oncologist takes the first call during after-hours and on weekends.
Care coordination with other providers
CBCCA has written policies and procedures to provide timely communication for referring providers and primary care physicians (within 72 hours). The time to respond and communicate with referrals is monitored by periodic audits. Comprehensive care plans are shared at multidisciplinary tumor board meetings weekly with primary care providers and other physicians involved in patient care.
Electronic Health Records
Our EHR system is certified by the Office of the National Coordinator for Health Information Technology (ONC), and has been in place since 2006. We completed 3 years of CMS’s meaningful use Stage 2 attestations. We have an active patient portal with secure bidirectional communication capabilities between patients and physicians, allowing patients to access their care plans. As part of meeting OCM standards, we will be upgrading our EHR system to add reporting capabilities.
Internet access
Our patient portal is active and accessible through smartphones; it enables a secure communication with patients about their care.
Patient navigators
The primary function of a patient navigator is to facilitate access to emergent and urgent care. Our patient navigators primarily have a nursing background and are trained in symptom management pathways, such as neutropenia, chemotherapy-induced nausea and vomiting, deep-vein thrombosis (DVT), pulmonary embolism (PE), and other side effects related to cancer treatment.
Patient navigators play a key role in managing side effects to reduce the number of emergency department visits and hospitalizations. In addition, they are trained in finance and economics, as well as in linguistically and culturally sensitive communication that is confidential, respectful, compassionate, and mindful of the patient’s safety issues. The hospital-based navigator is in place and is accessible.
Care plans
Care plans are shared with patients via the EHR and paper copies at the end of each office visit. They include the following details:
- Patient information
- Diagnosis, pathology, and disease stage
- Prognosis and treatment goals
- Initial plan for treatment and proposed duration, including specific chemotherapy drug names, doses, and schedule
- Expected response to treatment
- Treatment side effects, toxicities, and risk–benefit profile
- Quality of life and patients’ likely response to treatment
- Psychosocial health needs
- Advance care plans, including advance directives and other legal documents
- Survivorship plan, including a summary of treatment and information regarding recommended follow-up activities and surveillance, as well as risk-reduction and health promotion activities
- Care team and coordination
- Financial information regarding the total and out-of-pocket costs of treatment.
National Guidelines and Choosing Wisely
Our care management pathway and navigation function will allot resources to address the aspects of care that are the most common reasons for emergency department visits and hospitalizations, with a proper triage system and navigation to allow patients who receive active treatment to have direct access to infusion and consulting services. These services, combined with in-house laboratories and radiology amenities, will reduce avoidable emergency department visits and hospitalizations while improving patients’ and caregivers’ quality of life. Six of our employees have completed an oncology navigator certification course.National guidelines
Patients receive treatment according to the NCCN/ASCO guidelines. In the next 6 months, we will be developing data-mining capabilities to identify adherence to guidelines and the reasons for nonadherence.
Choosing Wisely
We are actively pursuing the implementation of choosing appropriate tests and supportive care pathways (eg, growth factor use, frequency, and type of imaging) based on ASCO’s recommendations. We are also developing data-mining capabilities to monitor adherence to the Choosing Wisely recommendations.
Symptom management pathways
We have symptom management pathways for chemotherapy-induced nausea and vomiting, dehydration and fatigue, neutropenic fevers, DVT and PE, depression, and constipation and diarrhea. The addition of patient navigators and a dedicated triage nurse should reduce emergency department visits and hospitalizations.
Compliance measurement through EHR
Our ONC-certified EHR system completed the meaningful use Stage 2 attestations for 3 years. Our system will be upgraded (at a reasonable cost) to meet the OCM reporting requirements.
Primary and secondary prevention
We recruited a dietitian and a nutritional counselor to help patients who are at high risk for relapse as a result of increased body mass index and other obesity-related conditions.
In addition, we plan to recruit a health coach to integrate nonpharmacologic lifestyle modifications, such as exercise and other evidence-based interventions for a healthy lifestyle. We will implement a cancer prevention education series for the prevention, screening, and early detection of other diseases for patients diagnosed with a specific type of cancer.
In terms of ancillary diagnostic services, we have a computed tomography scanner for immediate access and cost-efficiency, and a full-service complete blood count unit and anticoagulation monitoring services. In addition, we established in-house molecular diagnostic services, such as immunophenotyping and flow cytometry, to assist in the diagnosis of hematologic malignancies. We are also adding screening for pain medications, because frequent monitoring is recommended by the Drug Enforcement Administration and by the state legislature.
Palliative and end-of-life care
We have a board-certified hospice and palliative care physician to assist in end-of-life care. We also have a voluntary lay chaplain to assist in the spiritual care of patients.
Conclusion
Our pursuit of practice transformation has yielded many benefits for all our stakeholders. Patients experience the benefits of patient-centric care, greater care coordination and communication, a better-established relationship with their physicians, and real-time and on-demand access to care.
Our physicians experience the benefits of standardization of the science of medicine, practice revenue stabilization, improved efficiency, and standardized data compilation.
Payers benefit from a reduction in cancer spending, increased patient engagement, care that is appropriate to the patient’s condition, and a focus on the reduction of avoidable complications.
Although this transformation was time-consuming, resource-intensive, and, at times, seemed unachievable, on completion of the transformation and becoming the first NCQA-accredited patient-centered oncology practice in South Carolina, we have been able to negotiate reimbursement for additional nonevaluation and management cognitive services, as well as for weekend services.
We believe that the PCSP accreditation helped us improve the quality of patient care, reduce unnecessary costs driven by avoidable factors, and position the practice on the path to a patient-centric experience. When CMS announced the new OCM model, the application process, selection, and transition into a fully functioning OCM site appeared achievable and readily acceptable to all our providers.
Acknowledgments
We would like to acknowledge the employees and physician owners of the practice for their help and contribution in successfully transitioning CBCCA. In addition, we would like to express gratitude to Arya Patel, Jeff Berwager, Radhika Kothadia, Resha Kodali, Seema Shukla, and Saheli Parekh for their help in this transition process.
For questions related to this article, contact