Cancer care expenditures in the United States are staggering, and are only expected to climb. In 2010, the total cost of cancer care was $125 billion.1 By 2020, with more individuals living with cancer as a chronic disease, costs are expected to grow by 39% and exceed $170 billion.1 Faced with this dramatic escalation of costs, providers, commercial payers, and the government are testing different methodologies for reimbursing cancer care. The aim is to shift the economics from a fee-for-service environment (ie, buy and bill) to one that rewards quality, efficiency, and a lower cost of care (Figure 1).
The full transition to value-based reimbursement will likely be one of trial and error. To date, many reform activities have targeted operational processes and practices as indicators of quality. In certain markets, payers have started to partner with providers to experiment with sharing the risk of patient care costs. Unlike the larger patient panels in primary care settings, cancer care is challenged by smaller patient cohorts with increased risk from cost variability. Many of the early cancer reimbursement pilots have evaluated different measures to account for the complexity and corresponding risk in cancer care.
Just recently, the US Department of Health & Human Services announced a new Oncology Care Model, applicable to beneficiaries who are undergoing chemotherapeutic regimens.2 This per-beneficiary, per-month payment model, with potential incentive payments for demonstrated cost-savings, is the latest example of the transition toward reimbursement models that focus on value.
From an oncologist’s point of view, the patient care, operational, and financial implications will need to be understood before any new reimbursement model is tried in daily practice. Certain practice characteristics, such as information technology (IT) system functionality or the local payer mix, can determine the success a practice may have utilizing one or all of these methodologies.
Payment Reform Overview
Throughout the United States, payers and oncology providers are collaborating on 4 types of value based reimbursement models:
- Pay for performance: performance-based payments related to the oncologists’ compliance with select clinical pathways and evidence-based protocols
- Oncology medical home (OMH): coordinated payments for care management across a spectrum of clinical and supportive-care services
- Bundled payments: episodic care payments designed to drive integration, quality, and efficiency through shared incentives and accountability
- Shared savings programs: targeted emergency department visit and hospital utilization cost reductions through adherence to clinical pathways and guidelines, with cost- savings to the payer and shared with the oncologists through reduced use of services and improved care management.
Certain pilots and initiatives in the United States have focused on one or more of the methodologies noted above. Each initiative seeks to test certain interventions and determine the impact on the cost of cancer care. Given this environment, it is important to ask whether your practice or center is ready to assume the challenges and responsibilities of participating in an alternative payment model. To help you answer that question, each model and relevant examples are discussed below.
Pay for Performance
Pay for performance rewards the quality of care through payment incentives for value, with value broadly defined as a function of quality, efficiency, safety, and cost. This incentive-based approach usually produces results on select measures, but it may not address all areas that a payer, employer, patient, or healthcare delivery system would like to monitor. In oncology, payers typically reward providers who adhere to evidence-based protocols and clinical pathways.
The Innovent Oncology program (supported by McKesson Specialty Health and US Oncology Inc), Texas Oncology, and Aetna explored an oncology payment model that highlighted the importance of evidence-based protocols.3-5 These organizations sought to change certain cost drivers within cancer care, specifically the variable use of drugs, the deterioration of patient health between treatments, and patient acceptance of interventions near the end of life.3-5 The 2-year pilot project focused on the following5:
- Provider use of evidence-based clinical pathways and health IT
- Patient support services
- Advance care planning (ACP).
Aetna incentivized provider adherence to the evidence-based guidelines and ACP. Health IT systems supported physician access to and use of the guidelines and allowed for information sharing and performance monitoring across the group. Oncology nurses worked with the practices and the Aetna care management team to help patients manage treatment symptoms and side effects. Finally, patients were offered access to end-of-life planning throughout their care. The results included improved pathway adherence from participating providers. In a recent article on the outcomes of this pilot, cost reductions from a decline in emergency department visits, hospital admissions, and the number of hospital days were more than $500,000 for the 221 pilot members.5
As a pilot, the Aetna example was successful in demonstrating the value of incentivizing performance, with performance defined as pathway adherence. The challenge to an oncology provider is that, historically, limited incentives have been linked to pay-for-performance methodologies. To fully evolve from a fee-for-service model, pay-for-performance initiatives will need to be included with other value-based reimbursement models.
Oncology Medical Home
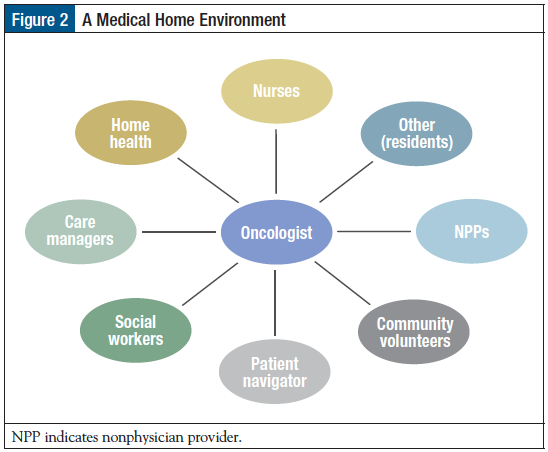
An OMH is designed to improve quality and reduce the waste that results from poorly coordinated care. The transition to a medical home model in primary care practices generally reorients the care model from a single provider to a coordinated team that shares information among clinicians and specialists (Figure 2). This concept is not new to cancer care practices, and cancer centers typically organize care in a patient-centric manner, which includes patients and their families or other caregivers in planning care and managing conditions. The National Committee for Quality Assurance (NCQA) certifies primary care and specialty practices that meet the organization’s requirements for focusing on the patient and coordinating care.6
A notable pilot is the COME HOME project,7 in which several community oncology practices are participating. In addition to that initiative, Consultants in Medical Oncology and Hematology, PC, a 9-physician medical-oncology practice, reengineered its care delivery processes and became the first NCQA recognized level 3 Oncology Patient-Centered Medical Home (PCMH). For payers and providers, the aims of a PCMH program are enhanced adherence to evidence-based protocols and a targeted reduction in the total cost of care.
Some PCMH models may include provisions for sharing savings between payers and providers that are achieved from better disease management. Others may embed upfront payment in the form of a care coordination or patient navigation fee or similar compensation to support additional resources for more comprehensive patient support. This fee, or per-member per-month (PMPM) payment, needs to be evaluated to project the incremental revenues and expenses to the practice or center. In many of the oncology projects, grant dollars were also included to support the additional expense within the practices. As these projects continue to gain traction with commercial payers, the PMPM payment will need to effectively compensate practices for these additional expenses and the evolution away from fee-for-service economics.
Bundled Payments
Bundled payments, also known as episode payments, encompass only certain services (eg, hospital inpatient and select physician services) or a part of the care continuum. In these bundled arrangements, a healthcare provider is given a lump sum that covers those specific healthcare services related to a specific diagnosis or procedure. The primary goal of bundling is to restructure financial incentives; these payments have generally been applied to conditions with a clear beginning and end.
UnitedHealthcare has piloted episode payments in the outpatient oncology setting to separate practice income from drug sales. The initiative was effective in reducing costs associated with certain medications, and established an environment of performance measurement and improvement. Recently, this payer signed a fixed payment agreement with The University of Texas MD Anderson Cancer Center for patients with a specific type of head and neck cancer.8 Several other initiatives with different payers have targeted specific modalities such as radiation oncology. Overall, bundled payments for a patient’s total cycle of treatment—and not the number of visits or the amount of chemotherapy given—may be conducive to patient-centric, evidence-based care that does not introduce conflicting revenue incentives for physicians.
Despite these efforts, it is important to note that bundled payments in oncology often can be difficult because of the complexity of cancer care; the various modalities, treatments, specialties, and sites of care make it difficult to define qualified patients for a specific episode of care. This complexity also impacts the payment allocation, requiring rigor in measuring, monitoring, and rewarding individual providers for quality and outcomes.
Recently, more discussion in the oncology community has targeted radiation therapy as the better treatment modality for bundled payments. Again, select pilots have been engaged across the country, with several larger radiation oncology practices promoting the benefits of bundled payments. This area will likely be one of continued interest as access to data, shared results, and community-based health information exchanges allow for the tracking of patients under this type of methodology.
Shared Savings Programs
When providers and health systems typically discuss shared savings initiatives, they usually involve accountable care organization participation under the Centers for Medicare & Medicaid Services’ Medicare Shared Savings Program (SSP).9 The focus of SSPs has not been cancer care; rather, high-volume chronic conditions, such as diabetes, asthma, heart disease, and chronic obstructive pulmonary disease, have been targeted. In light of the increasing costs of cancer care, commercial payers are working with oncology groups to pilot a range of shared savings initiatives that could change the economics of practices.
As an example, Priority Health, a regional, Michigan-based insurance carrier, spearheaded a 2-year OMH program in February 2011. Developed and implemented in collaboration with community oncology practices, the program currently encompasses more than 60 physicians in 6 practices and exemplifies the core elements of payment reform, care redesign, and performance measurement.10
First, the practices agreed to adopt the key elements of an OMH model: adherence to clinical pathways; enhanced patient education, engagement, and triage initiatives; ACP; and survivorship planning. As part of the agreement, the practices and Priority Health adopted performance metrics to assess patient experience, health outcomes, and per capita utilization. Early results included a decrease in emergency department utilization and a reduction in the total cost of care.
To align reimbursement with these value-based initiatives, Priority Health agreed to the following payment mechanisms:
- A monthly chemotherapy management fee
- Enhanced drug acquisition costs
- An annual infrastructure payment
- Enhanced fees for ACP, treatment planning, genetic counseling, and other agreed-on services
- Shared savings for reductions in emergency department visits and admissions.
Working with the practices, the payer recognized that to sustain change, several payment mechanisms were needed to achieve the agreed-on patient care goals in the most cost-effective manner.
Key Takeaways
Although there has been longstanding discussion about new models for healthcare delivery and payment reform, the conversation in oncology has rapidly turned to questions of “when” and “how,” rather than “if.” Simply acknowledging the evolving landscape will do little to help oncology providers in preparing and positioning themselves for the transitions ahead. Results from early programs have shown that the application of 1 or more of these reimbursement models has made an impact on the costs of delivering care to patients with cancer. Oncology practices will need to consider these new arrangements as well as the implications to their practices and patients.
References
- Mariotto AB, Yabroff KR, Shao Y, et al. Projections of the cost of cancer care in the United States: 2010-2020. J Natl Cancer Inst. 2011;103:117-128. Erratum in: J Natl Cancer Inst. 2011;103:699.
- Centers for Medicare & Medicaid Services. Oncology Care Model. http://innovation.cms.gov/initiatives/Oncology-Care/. Accessed March 6, 2015.
- McKesson Specialty Health-Innovent Oncology. Connecting payers and physicians for improved patient care. www.innoventoncology.com/web. Accessed March 6, 2015.
- McKesson Specialty Health-Innovent Oncology. Aetna and US Oncology team up to improve quality, cost of cancer care. www.innoventoncology.com/web/1AboutInnoventOncology/2News_Updates_ Archives/870C7B000C6B3855E0440003BADBF04B. Accessed March 6, 2015.
- Hoverman JR, Klein I, Harrison DW, et al. Opening the black box: the impact of an oncology management program consisting of level I pathways and an outbound nurse call system. J Oncol Pract. 2014;10:63-67.
- National Committee for Quality Assurance. Patient-centered specialty practice: excellence in care coordination, recognized. www.ncqa.org/Portals/0/Programs/Recognition/PCSP/PCSP_brochure.pdf. Accessed March 6, 2015.
- COME HOME: Innovative Oncology Business Solutions, Inc. The COME HOME model. www.come homeprogram.com/index.php/come-home-practices/. Accessed March 6, 2015.
- The University of Texas MD Anderson Cancer Center. MD Anderson, UnitedHealthcare launch new cancer care payment model. www.mdanderson.org/newsroom/news-releases/2014/md-anderson-unitedhealthcare-new-cancer-payment.html. Accessed March 6, 2015.
- Centers for Medicare & Medicaid Services. Shared Savings Program. www.cms.gov/Medicare/Medicare-Fee-for-Service-Payment/sharedsavingsprogram/index.html?redirect=/SharedSavingsProgram/. Accessed March 6, 2015.
- Fox J. Lessons from an oncology medical home collaborative. Am J Managed Care. 2013;19:SP5-SP9.